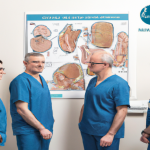
- Cutting-edge urology: Where science meets health. This photo depicts urologists engaged in groundbreaking research and application, pushing the boundaries of medical science for better patient care.
- Expert urologists consulting in a modern clinic, utilizing the latest medical advancements to offer personalized care. Their dedication to men’s health is evident in their focused discussions and patient-centric approach.
- Women’s Urological Health
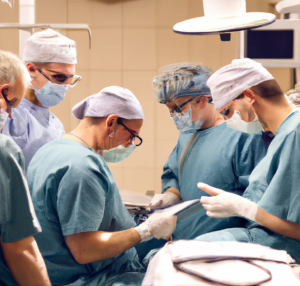
- Advanced urological care in action, showcasing a team of skilled professionals using state-of-the-art equipment to diagnose and treat complex conditions, ensuring every patient receives the best possible care.
- victoria urologists
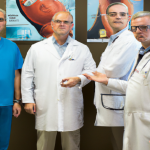
- The face of modern urology: An expert care team, united in their mission to advance men’s health through evidence-based practices and compassionate care.
- Dedicated urologists at work in a clinical setting, displaying their commitment to providing top-tier urological health services, with patient well-being as their top priority.
- Innovative urology: Blending cutting-edge technology with unparalleled expertise. Here, specialists are seen leveraging the latest medical advancements to revolutionize patient treatment and care.
Frequent Urination
The desire to use the restroom more often than normal, sometimes urgently, is known as frequent urination, and it may cause disturbances to sleep and everyday routines. This symptom may indicate to the body that there is an imbalance. To successfully manage this symptom, one must comprehend its processes and causes.
The intricate relationship between the kidneys, bladder, and nerve system powers the urine system. Urine is produced by the kidneys and stored in the bladder after they filter waste from the circulation. Nerve impulses suggesting the desire to pee are delivered to the brain as the bladder fills. Adults typically urinate four to six times a day, although there are a number of variables that might make this frequency higher.
Urine production may rise for a number of non-urological reasons. For instance, the body may create more pee if it consumes a lot of fluids, particularly those that include alcohol or caffeine. Due to their diuretic properties, these drugs cause the body to urinate more often, which throws off the fluid and electrolyte balance.
Frequent urination and the body’s ability to control blood sugar levels might sometimes be linked. The kidneys try to eliminate extra sugar from the body via urine when blood sugar levels are high, which results in more urine being produced. This procedure emphasizes the kidneys’ function in preserving homeostasis, or the physiological equilibrium of the organism.
The frequency of urine may also be influenced by hormonal fluctuations, especially in women. For example, hormonal changes during pregnancy, together with the increasing pressure of the uterus on the bladder, might result in more frequent visits to the restroom. In addition, variations in estrogen levels during menopause may impact the urinary tract’s health and functionality, resulting in increased urination.
While being hydrated is crucial, it’s also critical to match your body’s fluid requirements to avoid overstuffing your bladder. When the body strives to regulate salt levels, foods heavy in salt may cause water retention, which in turn increases urine output.

Pioneering urological treatments and solutions being discussed by top medical professionals, demonstrating their commitment to innovation and excellence in patient care.
Urinary Incontinence
Many people, particularly women, suffer from urinary incontinence, which is the involuntary leaking of urine. It may be uncomfortable and embarrassing, which might lower one’s quality of life. It is a symptom rather than the actual sickness. Urinary incontinence may be classified into many categories, each with unique causes and treatments.
One of the most prevalent types of incontinence, stress incontinence, is brought on by bodily movements or activities that increase pressure on the bladder, such as lifting, exercising, sneezing, or coughing. It is often associated with a weakening of the pelvic floor muscles, which manage urine discharge and support the bladder.
An abrupt, strong need to pee followed by an uncontrollably large loss of urine is the hallmark of another common kind of incontinence: urge incontinence. This disorder is often linked to hyperactive bladder, in which the muscles of the bladder contract excessively or suddenly, resulting in incontinence and frequent urine.
Making lifestyle changes and engaging in pelvic floor exercises to improve the muscles supporting bladder function are frequently the first steps in managing urine incontinence. Urinary retention and release may be greatly improved with regular, focused exercise, which lowers the risk of leaks.
Managing incontinence also involves a diet. Urging and the frequency of urine may be increased by certain meals and drinks that irritate the bladder. The symptoms may be lessened by cutting back on irritants like alcohol, coffee, and acidic meals.
Specialized therapies are available for those whose incontinence does not improve with conventional procedures. These may be anything from medical gadgets that help the bladder or urethra stay in place to more sophisticated procedures like surgery that improve bladder support or fix underlying anatomical problems.
Urology with a personal touch: Patient consultations. This image shows the warm, patient-centered environment where individual needs and concerns are addressed with care and professionalism.

Focused urology experts in a clinical conference, deeply engaged in exchanging knowledge and insights to stay at the forefront of urological medicine.
Urinary tract infections
Due to women’s shorter urethras, which make it easier for germs to enter the bladder, urinary tract infections (UTIs) are among the most common clinical diseases. Although the kidneys, ureters, bladder, or urethra may all be affected by a UTI, the bladder and urethra are more often affected. Early identification and care depend on an understanding of the symptoms, causes, and preventative actions.
Urinating more often without passing much pee, feeling as if you need to urinate right away, and experiencing a burning sensation when you urinate are all indicative of a urinary tract infection (UTI). More serious symptoms, including back pain, fever, and nausea, might appear when the infection affects the kidneys, signaling the need for immediate medical attention.
Underlying UTIs are bacteria, mainly Escherichia coli (E. coli), which are present in the digestive tract. The urethra, the bladder, and the anus are the possible migration points for these bacteria, which grow and infect the bladder. Moreover, germs may enter the urinary system during sexual activity, raising the risk of UTIs.
In order to lower the risk of UTIs, prevention techniques are essential. Drinking plenty of fluids, particularly water, helps dilute urine and promotes frequent urination, which helps eliminate germs from the urinary system before an illness can start. Hydration is thus crucial. There is conflicting data supporting the claim that cranberry juice may prevent UTIs; however, it does contain some compounds that may inhibit bacteria from adhering to the walls of the urinary tract.
Additionally important in avoiding UTIs are good personal hygiene habits. Bacteria from the anal area do not go towards the urethra when one wipes from front to back after using the restroom. Furthermore, it might be beneficial to urinate soon after sexual activity in order to remove any germs that may have entered the urethra.
It may be suggested to make lifestyle changes and have a conversation about using preventive measures under medical supervision for those who often have UTIs. The importance of prophylaxis cannot be overstated, as recurring infections may result in more severe problems.

Pioneering urological treatments and solutions being discussed by top medical professionals, demonstrating their commitment to innovation and excellence in patient care.

Urologists collaborating for better men’s health. This scene captures the essence of teamwork in medical practice, combining diverse expertise for comprehensive patient care.

Urological Associations
Pelvic Pain
A number of disorders affecting the reproductive, digestive, or urinary systems, as well as sometimes the musculoskeletal components in the pelvic region, may cause pelvic discomfort. Ignoring this symptom is advised since it may be a sign of underlying health problems that need urgent treatment or ongoing care.
The way that people feel pelvic pain varies greatly; it may be as mild and persistent as an ache or as severe and searing. Its strength might vary, and it can be confined to a single spot or dispersed across the pelvic area. The discomfort may be linked to certain behaviors, like peeing or having sex, or it may manifest itself without reference to any clear cause.
Pelvic discomfort may be caused by many circumstances. When it comes to the urinary system, disorders like bladder infections or stones may be quite uncomfortable. Many people report the discomfort as a lower abdomen ache that becomes worse when they urinate, indicating that they should see a doctor to rule out any infections or blockages and treat them.
Menstrual cramps, ovarian cysts, and endometriosis are among the reproductive system diseases that are often linked to pelvic discomfort in women. Sharp pains during menstruation or persistent discomfort that interferes with everyday activities are only two of the symptoms that these illnesses may induce. In order to correctly identify and treat the ailment, it is imperative that people exhibiting these symptoms see a physician.
Personalized treatment strategies and a medical examination to determine the underlying reason are frequently necessary for the effective management of pelvic pain, which calls for a multidisciplinary approach. Depending on what is causing the pain, treatments might range from medicine and physical rehabilitation to, in some situations, surgery.
Pelvic pain may also be relieved by food and lifestyle changes. Frequent exercise, especially that which strengthens the muscles of the pelvic floor, may ease discomfort and enhance pelvic health in general. Furthermore, constipation may worsen pelvic discomfort; a balanced, high-fiber diet helps avoid this.
- Innovative urology: Blending cutting-edge technology with unparalleled expertise. Here, specialists are seen leveraging the latest medical advancements to revolutionize patient treatment and care.
- Urology Lifestyle Advice
- “Urology specialists engaged in deep discussion about patient care, highlighting their commitment to continuous learning and collaboration in the pursuit of better health outcomes for men.
- State-of-the-art urology facilities in use, illustrating the clinic’s investment in high-quality healthcare infrastructure to enhance diagnostic and treatment capabilities.
- Urologists collaborating for better men’s health. This scene captures the essence of teamwork in medical practice, combining diverse expertise for comprehensive patient care.
- Urology team in action: Enhancing men’s health through collaborative efforts, showcasing their dedication to delivering comprehensive and effective urological solutions.